Other uses for your donation
While most donated blood is used clinically, your donation could also save lives in less direct ways, such as developing an artificial liver.
The liver performs many important functions, such as: absorbing nutrients, detoxifying and removing harmful substances from the blood, breaking down food and converting it to energy, fighting infections, and making enzymes and proteins including those involved in blood clotting.
Liver failure kills more than 10,000 people in the UK each year and a transplant is the only curative treatment. But a shortage of livers means only 1,200 liver transplants a year are performed in the UK, leading researchers to explore alternative solutions.
Now researchers at University College London (UCL), supported by The Liver Group Charity, have developed a new, bioartificial liver called HepatiCan. It’s been developed using plasma sourced from donated blood. Some donations are not suitable for patient use but they can still be used, for example in research, to help save and improve lives: HepatiCan is one example.
Developing a treatment for liver failure
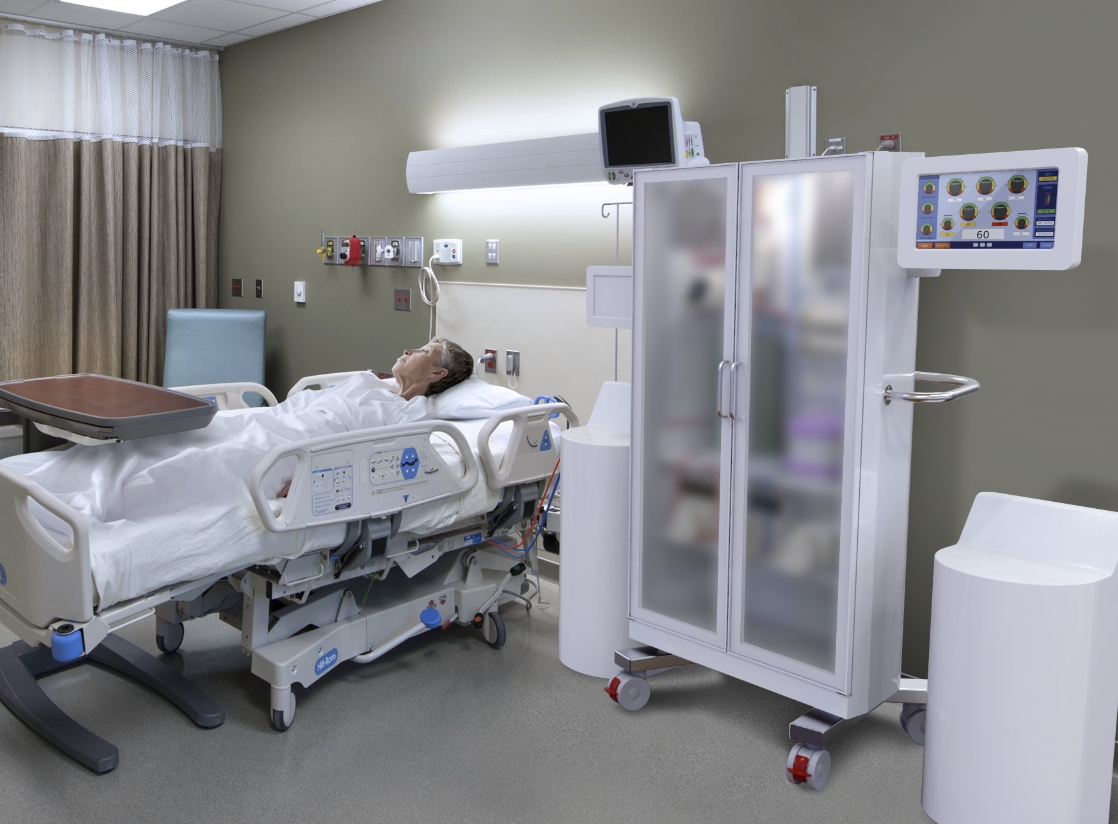 Given long enough, a damaged liver can repair itself. HepatiCan is a bioartifical liver machine that can give support to a patient, buying enough time for a failing liver to recover and regenerate. For many patients, this could mean avoiding the need for a transplant and would also make better use of scarce donor organs. During treatment, blood is taken from the patient’s body via an apheresis machine and is separated continuously into plasma and the cell fraction. The plasma is passed through the HepatiCan machine, which then removes harmful products. Healthy blood is then passed back to the patient.
Given long enough, a damaged liver can repair itself. HepatiCan is a bioartifical liver machine that can give support to a patient, buying enough time for a failing liver to recover and regenerate. For many patients, this could mean avoiding the need for a transplant and would also make better use of scarce donor organs. During treatment, blood is taken from the patient’s body via an apheresis machine and is separated continuously into plasma and the cell fraction. The plasma is passed through the HepatiCan machine, which then removes harmful products. Healthy blood is then passed back to the patient.
(Picture: Stylised image of HepatiCan)
The role of plasma
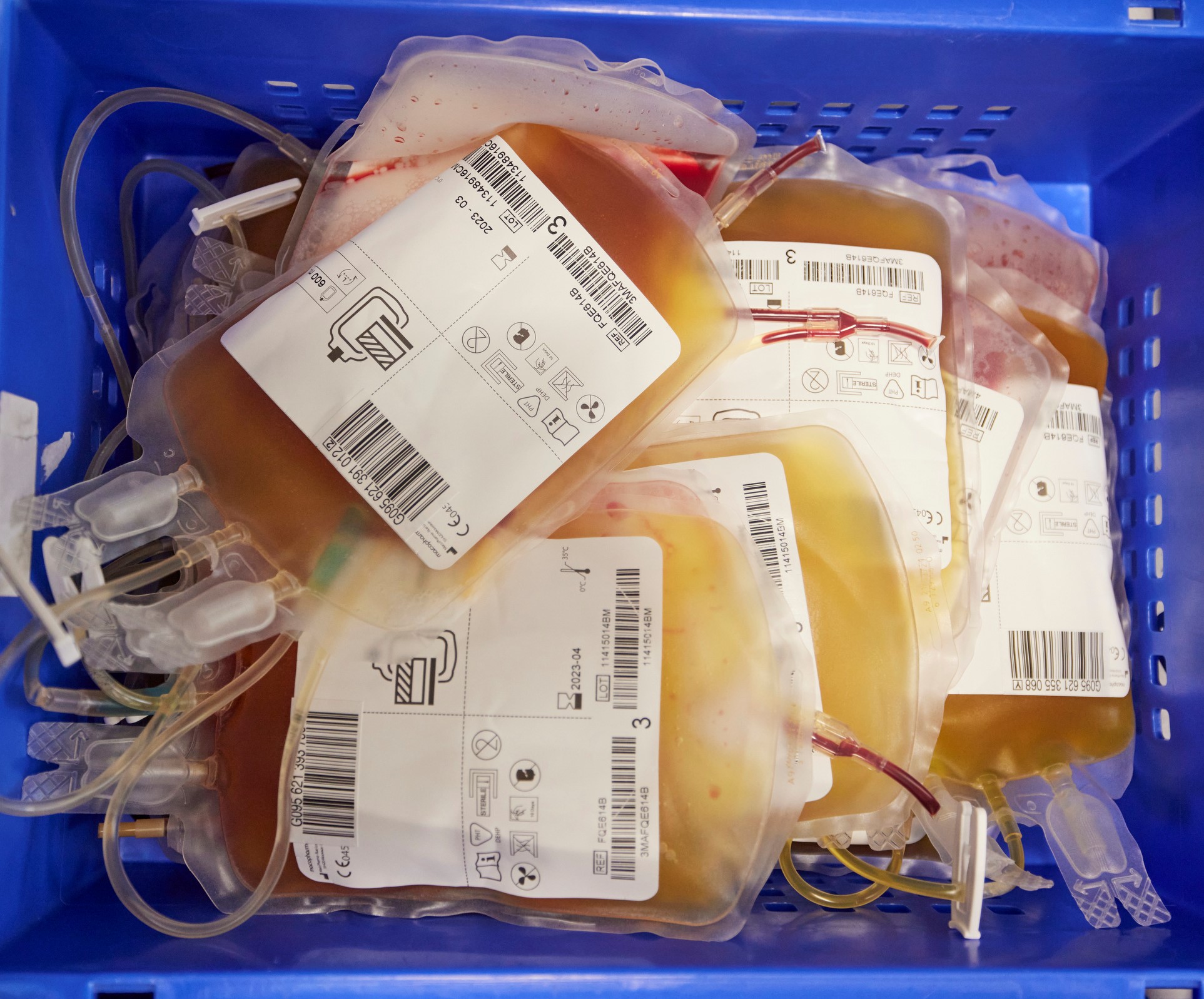 Plasma sourced from donated blood played and will play a fundamental role in the way HepatiCan was developed and how it works. Firstly, plasma is used to grow cell structures that mimic the liver. The machine contains around 70 billion liver cells. HepatiCan will be primed with human plasma before the patient is connected to the apheresis machine, which removes and processes the blood. It is important to use human plasma because the cell structures perform best in human plasma.
Plasma sourced from donated blood played and will play a fundamental role in the way HepatiCan was developed and how it works. Firstly, plasma is used to grow cell structures that mimic the liver. The machine contains around 70 billion liver cells. HepatiCan will be primed with human plasma before the patient is connected to the apheresis machine, which removes and processes the blood. It is important to use human plasma because the cell structures perform best in human plasma.
HepatiCan treatments could offer a patient the chance to return to their previous life after their liver repairs itself. Also, if patients don’t need a transplant, they don’t need lifelong immunosuppressants. Only patients for whom a transplant is the only option would then need a donated liver.
(Picture: Plasma from whole blood in the manufacturing centre)
The HepatiCan bioartificial liver, once ready, will be tested in a clinical trial for safety in three patients at the specialist liver transplant unit at UCL’s Royal Free Hospital campus. If the trial is successful, further clinical trials will take place to investigate its efficacy. After the trials, HepatiCan can be made ready for clinical use.
Non-clinical issue
 Through a service we call “non-clinical issue”, we provide blood to approved organisations for a range of approved work around the diagnosis and treatment of patients as well as the development of therapeutic products and services that could benefit patients in the future.
Through a service we call “non-clinical issue”, we provide blood to approved organisations for a range of approved work around the diagnosis and treatment of patients as well as the development of therapeutic products and services that could benefit patients in the future.
Why is blood surplus?
Some donations are unsuitable for clinical use because, for example, they are underweight or surplus to demand, or there are quality issues that mean the blood poses a potential risk to patients.
(Picture: Research scientist in the lab)
Who uses the surplus blood?
NHS Blood and Transplant policy and UK regulations cover the handling of blood and human tissue. Access to donated blood for non-clinical use is managed by a dedicated team within NHS Blood and Transplant. Clinical scrutineers ensure that each request is from an organisation with legitimate aims in line with donor consent, NHS Blood and Transplant policy and regulations (including ethical considerations).
Customers come from sectors including research, laboratory quality assurance schemes, medicine development, toxicology and validation for uses such as:
- Research into the latest advancements in medical treatments for illnesses and conditions such as COVID-19, cancer, arthritis, diabetes and many more
- Education and training
- Validating treatment and diagnostic services
- Production of blood test kits and test reagents
For more information about non-clinical use of blood, visit our website.

Donating plasma
Plasma is made into medicines that save and improve the lives of thousands of people with rare diseases.

Other stories
Remarkable stories from the world of giving blood – be they from the research lab, the hospital bed, or the donor chair
